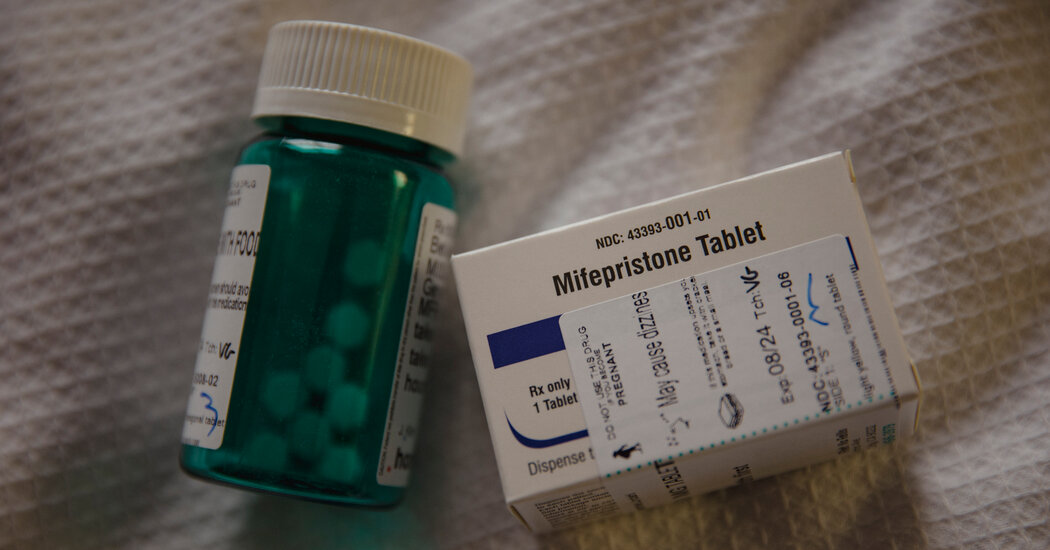
F.D.A. Advisers Say Benefits of Over-the-Counter Birth Control Pill Outweigh Risks
A panel of advisers to the Food and Drug Administration voted unanimously on Wednesday that the benefits of making a birth control pill available without a prescription outweigh the risks, a significant step in the decades-long push to make oral contraception obtainable over the counter in the United States.
If the F.D.A. approves nonprescription sales of the medication, called Opill, this summer, it could significantly expand access to contraception, especially for young women and those who have difficulty dealing with the time, costs or logistical hurdles involved in visiting a doctor, reproductive health experts say.
“I think Opill has the potential to have a huge positive public health impact,” said one advisory committee member, Kathryn Curtis, a health scientist with the Centers for Disease Control and Prevention’s division of reproductive health.
Approval is not a foregone conclusion, however. F.D.A. scientists who analyzed data submitted by the pill’s maker, HRA Pharma, raised concerns about whether women with medical conditions that should preclude them from taking the pill — primarily breast cancer and undiagnosed vaginal bleeding — would follow the warnings and avoid the product.
The agency’s reviewers also questioned whether a company study reliably demonstrated that consumers would follow the label’s directions to take the pill at roughly the same time every day and use another form of contraception or abstain from sex if they happened to miss a dose. The F.D.A. analysts also raised questions about whether younger adolescents and people with limited literacy could follow the directions.
“The F.D.A. has been put in a very difficult position of trying to determine whether it is likely that women will use this product safely and effectively at the nonprescription setting,” said Dr. Karen Murry, deputy director of the F.D.A.’s office of nonprescription drugs, during the advisory panel’s discussion session on Wednesday afternoon.
“We can’t just approve it based on the experience in the prescription setting without the applicant doing adequate studies to look at what’s likely to happen in the nonprescription setting,” she said. “But I wanted to again emphasize that F.D.A. does realize how very important women’s health is and how important it is to try to increase access to effective contraception for U.S. women.”
The advisory committee’s members overwhelmingly said that those concerns were vastly outweighed by the public health need in a country where nearly half of all pregnancies are unintended and by the long history of safety and efficacy of Opill, which was approved for prescription use 50 years ago.
“The panel expresses confidence in the effectiveness, not only in the general population of females, but also in adolescent populations and those with limited literacy,” said Maria Coyle, the chairwoman of the committee, a pharmacist and an associate clinical professor at Ohio State University. “The panel seems very comfortable with the limited number of risks from the medication itself.”
Several panelists said Opill might actually be safest for adolescents because they are very unlikely to have breast cancer, the main medical condition that precludes taking hormonal contraception.
“Adolescents really urgently need this,” said Dr. Leslie Walker-Harding, a panelist who specializes in adolescent medicine and the chief academic officer and senior vice president of Seattle Children’s Hospital. Young people often start off with contraception they can buy over-the-counter, and other such methods, including condoms, are much less effective than pills, which prevent pregnancy 93 percent of the time with typical use.
Most adolescents have “no or a lower efficacy of birth control methods available to them,” Dr. Walker-Harding said, adding that “this would dramatically increase the ability of kids not having unintended pregnancies.”
The panelists included obstetrician-gynecologists, adolescent medicine specialists, a breast cancer specialist and experts in consumer health behavior and health literacy.
Several said they believed few breast cancer patients would be at risk because their oncologists would advise them against using the pill. And many panel members who frequently prescribe birth control pills said that because doctors didn’t typically monitor patient adherence and often only saw such patients annually, there was no advantage to requiring a prescription.
Since the Supreme Court overturned the national right to an abortion last year, the accessibility of contraception has taken on more urgency. But even before that, the move to make a nonprescription pill available for all ages has garnered a groundswell of support from specialists in reproductive and adolescent health and groups like the American Medical Association, the American College of Obstetricians and Gynecologists and the American Academy of Family Physicians.
In a survey by the health care research organization KFF, more than three-quarters of women of reproductive age favored an over-the-counter pill, primarily because of convenience.
While some Catholic organizations have spoken out against over-the-counter birth control, most anti-abortion groups have been quiet on the issue. A vast majority of hundreds of comments submitted before the hearing supported approval of Opill. So did most of the 37 people who spoke during the hearing’s public comment portion on Tuesday, including young women who gave impassioned testimony about facing challenges obtaining prescription pills.
For proponents of over-the-counter pills, the main issue is affordability.
“This will not be a win if it is not affordable, covered by insurance and available to folks of all ages,” Kelly Blanchard, the president of Ibis Reproductive Health, said at a briefing on Monday organized by Free the Pill, a pro-over-the-counter coalition.
The Affordable Care Act requires only coverage of prescription contraception, and although some states have laws mandating coverage of over-the-counter methods, most states do not. The KFF survey found that 10 percent of women would not be able or willing to pay any out-of-pocket cost. About 40 percent would pay $10 or less per month, and about a third would pay $20 or less.
Frédérique Welgryn, the global vice president for women’s health at Perrigo, which owns HRA Pharma, said recently that the company planned to “make sure that the product is affordable to women” and that it would have a consumer assistance program.
Opill is known as a “mini pill” because it contains only one hormone, progestin, in contrast to “combination” pills, which contain both progestin and estrogen. A company that makes a combination pill, Cadence Health, has also been in discussions with the F.D.A. about applying for over-the-counter status.
HRA Pharma reported that participants in a study took Opill on 92.5 percent of the days they were supposed to take it. Most participants who missed a pill reported that they had followed the label’s directions to take mitigating steps such as abstaining from sex or using a condom, said Dr. Stephanie Sober, the company’s U.S. medical liaison. She said that among 955 participants, only six became pregnant while using Opill.
Most people who said they had missed doses attributed that to running out of pills before they could get to one of the study’s resupply sites, results that, Dr. Sober said, “illustrate precisely the barriers to adherence that could be lessened by switching Opill to the O.T.C. setting.”
But F.D.A. reviewers were concerned that about 30 percent of participants reported taking more pills than had been dispensed to them, a phenomenon called “overreporting” or “improbable dosing.” The reviewers wrote that “because the reported dosing was not possible, it leaves us with no clarity on what one-third of study participants actually took — or if they took any drug at all.”
Several advisory committee members said that the company’s data wasn’t perfect but that they were convinced that most people would use Opill appropriately and that the safety risks were low for those who did not.
“I think this represents a landmark in our history of women’s health,” said one panelist, Dr. Marjorie Gass, a retired obstetrician-gynecologist. “Unwanted pregnancies can really derail a woman’s life and especially an adolescent’s life. So I’m very pleased that the F.D.A. is seriously considering this, and I look forward to it being on the market.”